April 2026
Welcome to our April newsletter, the contents of which are as follows:
NEWS
Conference Summary: ‘Nourishing Our Future’: Turning Early Years Nutrition Guidance into Practice
New: Best Start in Life Family Hubs and Healthy Babies guidance
New: First Steps Nutrition Trust 2025 Impact Report
Infant milk news
ICYMI: Useful resources in light of recalls and price rises
BFLG-UK news
News: BMJ Article Raises Concerns About Formula Sponsored Survey Circulated by Midwifery Journal
Forthcoming
An update of First Steps’ Eating Well Healthy Start and Best Start Foods, a practical guide
The iHV Evidence Based Practice conference, Bournemouth, May 6th
The Unicef UK Baby Friendly Initiative virtual conference, virtual, November 18-19th
News
News: Launch of the Commercial Baby Food Review
We at First Steps Nutrition Trust are proud to announce that we have joined the Commercial Baby Food Review. Working alongside the Obesity Health Alliance, Bremner & Co, Sustain, Planetary Alliance and the University of Leeds. This new cross-sector initiative focuses on improving the nutritional composition and marketing of commercial baby and toddler foods in the UK, through stronger enforced regulations.
Funded by Impact on Urban Health, the Review brings together specialists in early years nutrition, food policy, public affairs, advocacy, public health and academia to drive population change with measurable benefits for child health and equality. The initiative will focus on tackling systemic inequalities in infant and young child feeding, including the disproportionate impact that unhealthy, inappropriate products and misleading marketing can have on low-income families.
The problems are not new, but they have long been ignored. Important new research published in the last year (summarised in our May 2025 newsletter) highlighted ongoing, serious concerns with the baby food retail offer. Key findings included:
Product Composition
Around a quarter of all products would need a front-of-pack warning for high sugar
41% of main meals were high in sugar
Cheaper options were often higher in sugar, more watery, and less nutritious, raising further concerns about affordability and inequalities
Labelling and Marketing
Every product carried nutritional or marketing claims
Many products labelled for use from 4 months of age, against public health recommendations
Parent Insight
92% of parents with children aged 0-3 use commercial baby and toddler foods
40% of parents with babies under 6 months use these products daily
The Review comes at a pivotal moment. With voluntary guidelines published in August 2025, the 18-month implementation period is well underway, and pressure is growing on manufacturers and retailers to make meaningful improvements. The Review will work to develop practical, evidence-informed policy solutions that strengthen accountability, support regulatory reform, improve the commercial baby food retail offer, and better protect babies’ and young children's health.
This opinion piece of ours in the Grocer “Baby food guidelines: Why we’re still waiting for real progress” highlights the need for sufficient scrutiny of baby food company actions in response to the voluntary guidelines.
You can read an interview about the Review, between our Director Vicky and Bremner and Co partner, Dayna Brackley here: “Baby pouches and health halos: the new partnership demanding better baby food”.
New: Food Foundation survey showing the multiple barriers families face feeding under 5s healthy diets
The Food Foundation published the results of their latest food insecurity monitoring in March (see here) and reported that 15.3% of households with children reported experiencing food insecurity in January 2026, compared to 10.9% for households without children. Food insecurity means having to have smaller meals or skipping meals, not eating when hungry, or having to go a whole day without eating because of being unable to access or afford enough food at any point in the past month.
Food insecurity impacts on nutrition, with the survey finding food insecure households reporting cutting back on purchases of fruit (53.1%) and vegetables (39.9%), which could in turn impact on the diets of young children and contribute to some of the inequalities in consumption. Dietary inequalities fuel rising levels of childhood obesity and persistently high levels of dental decay.
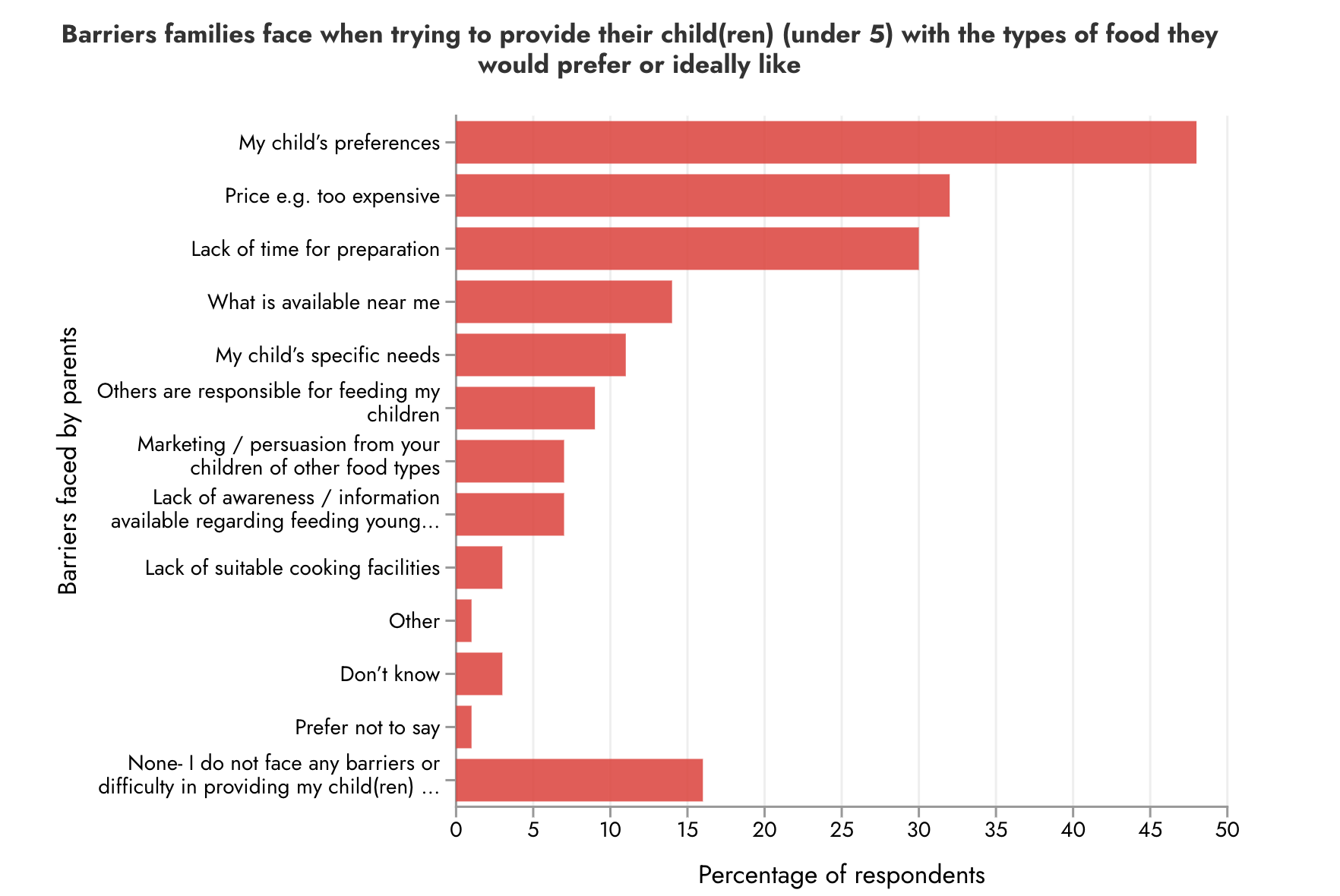
Nearly three quarters (74%) of survey respondents with children aged 1-4 years reported at least one barrier to feeding their child what they would like. The graph shows the multiple barriers reported by families of young children:
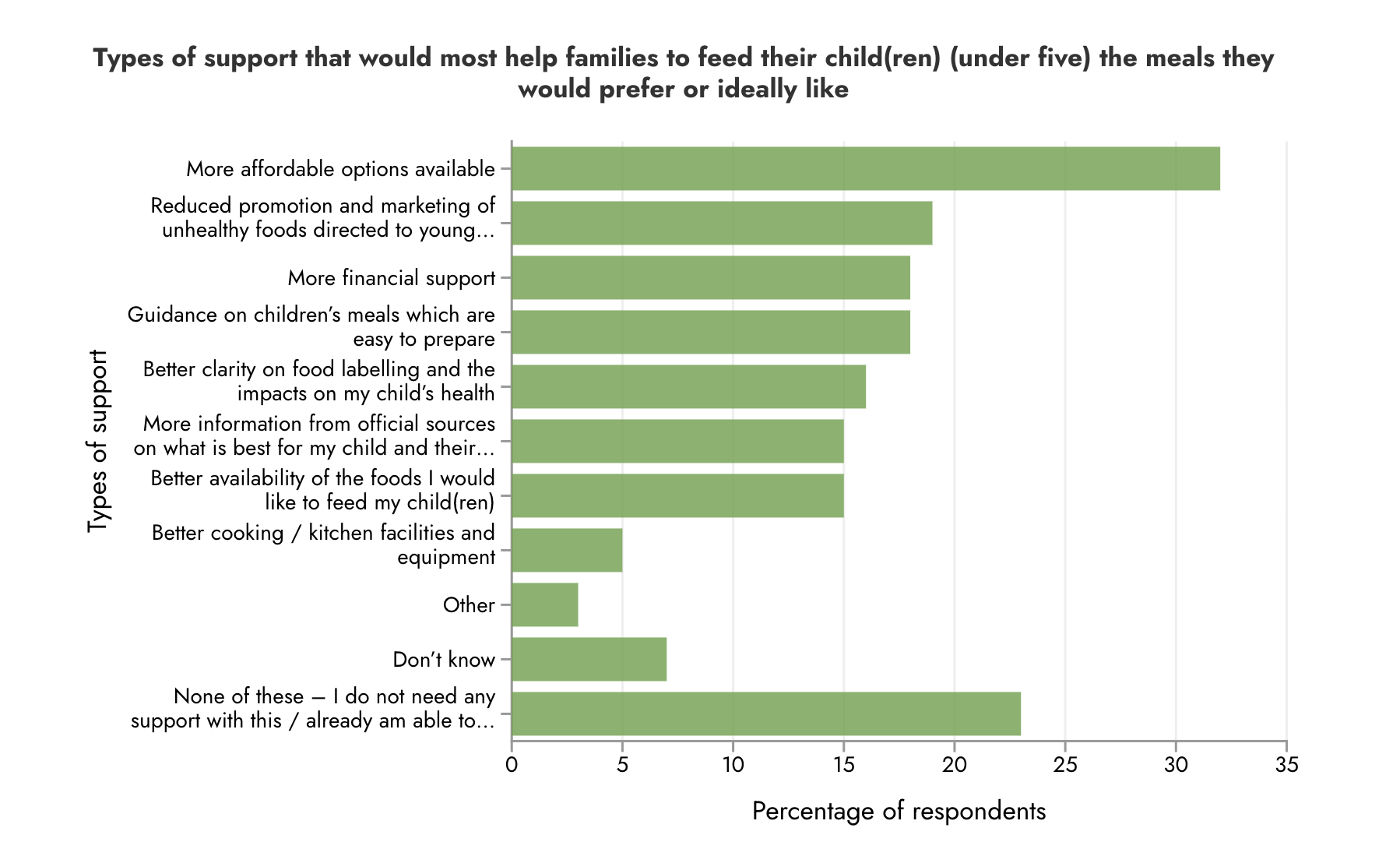
This graph shows what families said would help them to feed their young children better:
We back the Food Foundation’s calls for:
Improving the Healthy Start scheme (expanding eligibility to include children aged four, increasing the payment amounts to ensure it keeps in line with food inflation, and automatically registering all eligible families onto the Healthy Start scheme).
Improving Free Early Years Meals (removing additional conditions attached to eligibility).
Strengthening regulations on the promotion and marketing of unhealthy foods directed at young children (including mandating standards for commercial baby and toddler foods, as per our work on the Commercial Baby Foods Review, outlined above).
News: Investigation shows many branded, children’s vitamin D products do not contain enough vitamin D
On March 21st, the Times reported the results of an investigation in to branded, children’s vitamin D products which suggested that parents are being misled over dosages. The issue is that many supplements are labelled as meeting 100% of the ‘Nutrient Reference Value’ while containing less than the 10 micrograms of vitamin D that the NHS recommends is given to all children aged 1-<5 years daily (and to breastfed babies from birth, unless they are drinking 500ml or more formula a day).
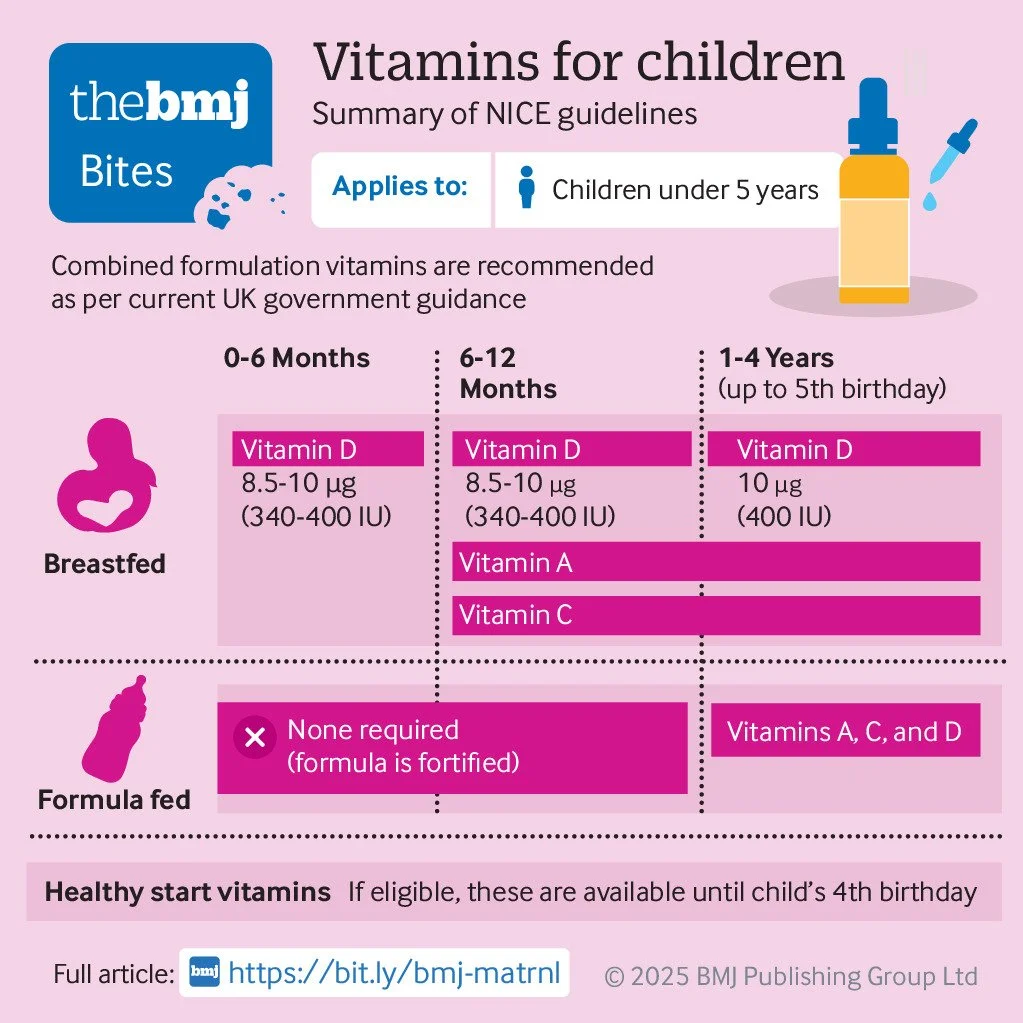
This infographic from the BMJ summarises current public health recommendations for vitamin supplements for babies and young children (nb. Healthy Start vitamins can be used from birth).
Key takeaways for parents of <5s and health workers supporting them:
Branded supplements are usually not the best choice, they come with a price tag, they may not provide what the child needs (as outlined in the infographic above) plus may add to excess sugar intakes
Pharmacy own-brand vitamin D supplements are usually the better choice
Healthy Start vitamins (providing vitamins D, C and A) provide the right doses, are FREE to eligible, low-income families (and all families of <4s in some areas) and can be bought online at low cost.
Our Eating Well guides provide practical guidance on feeding babies and young children under 5 years of age and include advice on vitamin supplementation. These guides can be access for FREE or a donation (and some can be bought as hard copies) from our main website, here: https://www.firststepsnutrition.org/eating-well-resources.
Conference Summary: Imperial Ultra-Processed Food Policy Forum -Assessing the science and advancing regulatory and policy responses to ultra-processed foods
Our Director, Vicky, was honoured to be among 15 distinguished speakers at this second UPF forum at Imperial College London on March 24th. The purpose of the event was to examine the latest evidence on Ultra-Processed Foods (UPFs) and to identify practical policy responses to their growing role in diets and disease.
Below are some highlights from Imperial’s Annabel Culley’s news piece on the event, and some extra detail from Vicky’s presentation.
The State of Evidence behind Ultra-Processed Food
Professor Carlos Augusto Monteiro gave the keynote, summarising the state of scientific understanding linking UPFs with ill health. He summarised and built on the Lancet series paper 1 published last year (read about this in our December 2025 newsletter), highlighting that the problem with UPFs lies not only in their nutritional profile, but in the very processes, ingredients and additive combinations used to manufacture them, which drive overconsumption and damage health through multiple pathways. He also addressed some of the criticisms of UPF research.
Dr Matilde Touvier presented her work on the mechanisms by which UPFs harm health.
Dr Ashley Gearhardt presented on the addictive properties of UPFs and how modern processing optimises sensory appeal and intensity, speed of delivery, and drives repeat consumption.
Dr Sam Dicken presented the UPDATE randomised controlled trial findings, comparing the health effects of two diets meeting the current UK national dietary guidelines, one UPF-based and one made of minimally processed foods.
UPF Policy Landscape
The second part of the conference focused on the direction of UPF policy research. Professor Adam Briggs introduced three new NIHR-funded research projects building the evidence base needed to develop and justify effective policy interventions in the UK. Thereafter, Professor Sassi, Dr Eszter Vamos and Dr Dan Derbyshire spoke about these three new projects and how findings will be translated into actionable policy recommendations. We at First Steps are collaborating on the project being led by Eszter (‘Identifying and evaluating policy mechanisms to reduce ultra-processed food consumption in the UK: health, equity and economic impacts’), along with friends at the Soil Association and Sustain’s Children’s Food Campaign
Dr Kremlin Wickramasinghe outlined the WHO’s current direction on UPF policy guidance, including work to establish internationally harmonised definitions and evaluate policy tools such as front-of-pack labelling, marketing restrictions, and taxation.
Dr Fabio Gomes of the Pan American Health Organisation presented evidence from Latin America, where countries including Brazil, Chile, and Mexico have implemented some of the most comprehensive food labelling and advertising regulations in the world.
Practical Steps to Action
In the afternoon, speakers including Vicky, spoke about specific policy levers available to governments seeking to reduce UPF consumption and improve diet quality.
Dr Austin Frerick spoke about anti-trust policies and institutional procurement to help break cartels and monopolies in the food system.
Dr Mathilde Touvier showed how front-of-pack labelling can empower consumers to identify and limit UPF exposure, while incentivising reformulation.
Dr Magdalena Muc presented evidence to show that loopholes in UK healthy food marketing restrictions need closing to limit young people’s exposure to UPF marketing.
And finally, our Director, Vicky presented on the policy options to rebalance early years diets away from UPFs, as follows:
Policies that seek to reduce UPF consumption in the early years:
Address processing in dietary guidelines and education as well as nutrients and foods
Restrict marketing of commercial milk formulas (and bottles and teats)
Mandate the International Code of Marketing of Breastmilk Substitutes in law, and properly enforce
Plain labels for infant formula
Tax unnecessary growing up and toddler milks and drinks
Restrict marketing of commercial baby and toddler foods
Update current laws in line with the WHO Europe Nutrient and Promotion Profile Model and UK public health recommendations (noting that while this would address many issues with the retail offer, additional work is needed to address texture, contaminants and additives)
Address UPFs in nutrition guidelines for early years settings (and school food) as well as nutrients and foods, e.g. explicit guidance to avoid commercial baby and toddler foods
Policies that seek to increase consumption of nutritious, minimally processed foods in the early years:
Ensure accessible, practical support for breastfeeding and legal protections (including adequate paid maternity leave)
Implement healthy food subsidy / nutrition safety schemes, e.g. Healthy Start
Ensure adequate practical support for complementary feeding based on nutritious minimally processed (requires adequate community health workers e.g. health visitors)
Mandatory food standards for early years settings, based on nutritious minimally processed foods
The Way Forward
Following the above presentations, Dr Dolly van Tulleken hosted a panel to investigate the gap between evidence and political action.
Ben Coleman MP emphasised that affordability and equity should remain a key focus in discussions around UPF policy. Baroness Walmsley stated that although the government has introduced a range of policies recommended within the House of Lords Report on Food, Diet and Obesity, the government need to go further and faster with its interventions.
Closing the conference, Henry Dimbleby concluded by highlighting the progress that has already been made, noting that 94% of people in the UK know that UPFs are bad for their health. He emphasised that the power lies in giving support for positive policies such as teaching cooking in schools and – reiterating the point Vicky made in her presentation - enabling breastfeeding.
To conclude, the forum highlighted growing international consensus regarding the growing evidence linking UPFs to poor health outcomes and how the policy debate is shifting from whether to act, to how to act.
Huge congratulations to the team at Imperial for a thought provoking and motivating day and for inviting us to share our expertise at the intersection of early years nutrition policy, practice and research and ultra-processed foods.
The presentations from the day can be watched on You Tube at this link: https://www.youtube.com/watch?v=Otuq6YRfLeU.
Conference Summary: ‘Nourishing Our Future’: Turning Early Years Nutrition Guidance into Practice
On 14th March 2026, our nutritionist Sara attended and exhibited the Nourishing Our Future (NOF) Conference, an inspiring event that highlighted the impact of the NOF on nutrition in early years settings across Essex.
What is Nourishing Our Future?
Nourishing Our Future began as a research programme focused on food and nutrition in early years settings, including nurseries, pre- schools, childminders and nursery classes caring for children from birth to age five. While the importance of nutrition in schools is well recognised, there has historically been far less focus on food in early years settings, despite its critical role in children’s growth, development and longer-term health.
The research was led by Anglia Ruskin University and commissioned by Essex County Council Public Health, who identified early years settings as a key priority within the county’s Healthy Weight Strategy (2024 to 2034), in light of local data showing that 21% of children aged 4 to 5 in Essex live with overweight or obesity, and 22% experience tooth decay. These challenges are closely linked to diet and dietary patterns established in early childhood.
Despite the existence of national guidance, the NOF research identified that early years settings often found it complex and difficult to interpret in practice. While many settings already had food policies in place, practitioners frequently reported uncertainty around portion sizes, menu planning, lunchbox expectations and how to engage parents confidently around healthy eating.
From Research to Action: The NOF Award
In response to the research findings, the NOF Award was developed in 2025 to support settings to turn evidence and guidance into action. It provides a clear, practical and supportive framework that helps settings understand what good practice looks like and how to implement it in a manageable way.
Through three progressive levels (Rooting, Sprouting and Blooming), the award supports settings to review and strengthen food and nutrition policies, improve menus, snacks and portion sizes, embed food education and positive mealtime experiences into daily practice, engage parents and carers using consistent, evidence-informed messages, and build staff confidence and shared responsibility around nutrition. It offers practical tools such as templates, training videos, example policies and family-facing resources, enabling settings to make realistic and sustainable improvements rather than expecting rapid or unrealistic change.
Impact and progress across Essex
The Nourishing Our Future Impact Report (2026) demonstrates that the programme is already supporting meaningful change across early years settings in Essex.
Engagement and Reach:
Over 200 early years settings participated in the original research, across all Essex districts.
Within the first six months of the NOF Award launch, 110 early years settings signed up, including childminders, nurseries and preschools.
10% of participating settings are located within the 20% most deprived areas in the country, demonstrating the programme’s reach into communities where food inequality is greatest.
33 settings achieved the Rooting level award during the early phase, with some settings progressing to higher award levels.
Changes in Practice:
83% of settings reported doing something differently because of taking part in the original NOF research.
91% of settings achieving the Rooting level award stated that they had changed their food and nutrition practices. Examples of change included revising snack menus, reducing sugar and ultra-processed foods, introducing clearer lunchbox guidance, improving portion control, and offering a wider variety of fruit, vegetables and home-cooked foods.
Confidence, Knowledge and Culture:
87% of settings reported improvements in staff knowledge, confidence and nutrition-related practice.
67% reported a positive shift in behaviour, attitudes and setting culture, with food becoming more central to wellbeing and learning rather than an operational afterthought.
All settings achieving the Rooting level award reported feeling much more confident in understanding and applying national nutrition guidance.
Impact on Children and Families:
73% of settings reported seeing a positive impact because of changes they had implemented.
Settings described children being more willing to try new foods, showing greater curiosity about food, and experiencing calmer, more positive mealtimes.
Many practitioners reported stronger engagement with parents and carers, including healthier lunchboxes, improved portion awareness and more consistent messaging between setting and home.
Reflections from the Conference
A strong theme throughout the conference was the dedication of early years professionals across a wide range of roles, including head teachers, managers and catering staff, all contributing to children’s food experiences and nutrition. Their commitment was celebrated alongside honest discussion of the financial, practical and emotional pressures faced by many settings.
Practitioners shared practical examples of change, from improved menus and food policies to creative ways of involving children and families in food education. It was clear that NOF has helped build shared understanding and confidence, supporting settings to prioritise nutrition while promoting positive, pressure-free relationships with food.
Implications for Future Policy
The NOF award has been presented as a best practice case study of how to implement the new National EYFS Nutrition Guidance (read more about this in our June 2025 newsletter) and has been shared with the Office for Health Improvement and Disparities, the Department of Education and the Local Government Association. NOF provides a strong example of how national ambitions, including the Best Start in Life agenda, the NHS focus on prevention, and local Healthy Weight strategies, can be translated into meaningful action in early years settings.
While funding and capacity vary across local authorities, the programme highlights the potential benefits of prioritising early years nutrition as part of a preventative public health approach that can help reduce health inequalities. Over time, such investment has the potential to support improved health outcomes for children and families and reduce longer-term pressure on health services, reinforcing the case for sustained and targeted support for early years nutrition at both local and national levels.
Find Out More
To learn more about the Nourishing Our Future programme, visit:
Website: https://nourishingourfuture.co.uk/about/
Facebook: https://www.facebook.com/share/g/1DqiemrLNs/?mibextid=wwXIfr
Instagram: https://www.instagram.com/nourishingourfuture/
Supporting Settings with Trusted Resources
Access to clear, impartial, evidence-based resources can further support early years settings to put guidance into practice. At First Steps Nutrition Trust, we provide practical resources that many settings and parents find helpful, including:
New: Best Start in Life Family Hubs and Healthy Babies guidance
On March 30th, the Department for Education issued new guidance to help local authorities provide Best Start Family Hubs and Healthy Babies services from April 2026 to March 2029.
As promised in “Best Start Family Hubs and Healthy Babies: preparing for implementation from April 2026” published in December 2025, the new guidance comprises:
Best Start Family Hubs and Healthy Babies: guidance for local authorities
Best Start Family Hubs and Healthy Babies: wider service expectations
The first two documents contain content related to infant feeding (i.e. breastfeeding and formula feeding) and (a small amount of information on) healthy growth and nutrition support. (Curiously there is no explicit mention of supporting families with complementary feeding or indicators related to this, which seems like an important omission which we will follow up on with the Department of Education).
Infant Milk News
Updated: Infant milk costs and trends reports
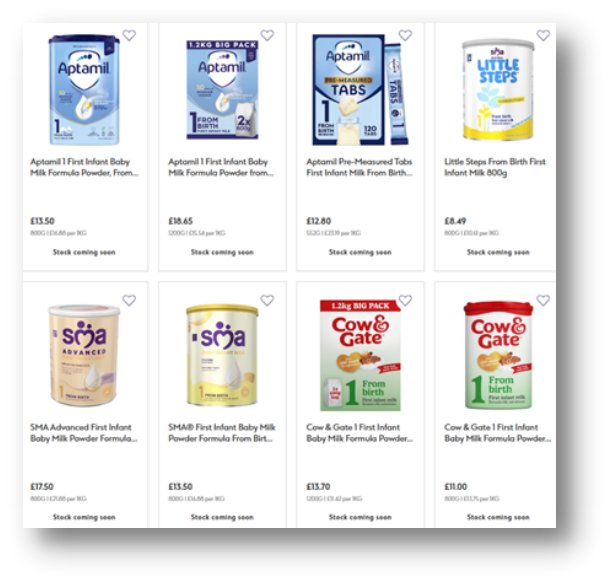
At the end of February, we published updated costs and trends reports as an additional update to our usual biannual releases in May and October. We did this in response to sharp price increases following the recent formula milk recalls (see below). Parents and carers quickly felt the impact, with one reporting on social media that Cow & Gate rose from £9.20 to £11 in a single week. Our findings were reported on by The Sun, The Grocer and the BMJ. Beyond pricing, the recent recalls also disrupted availability (see below).
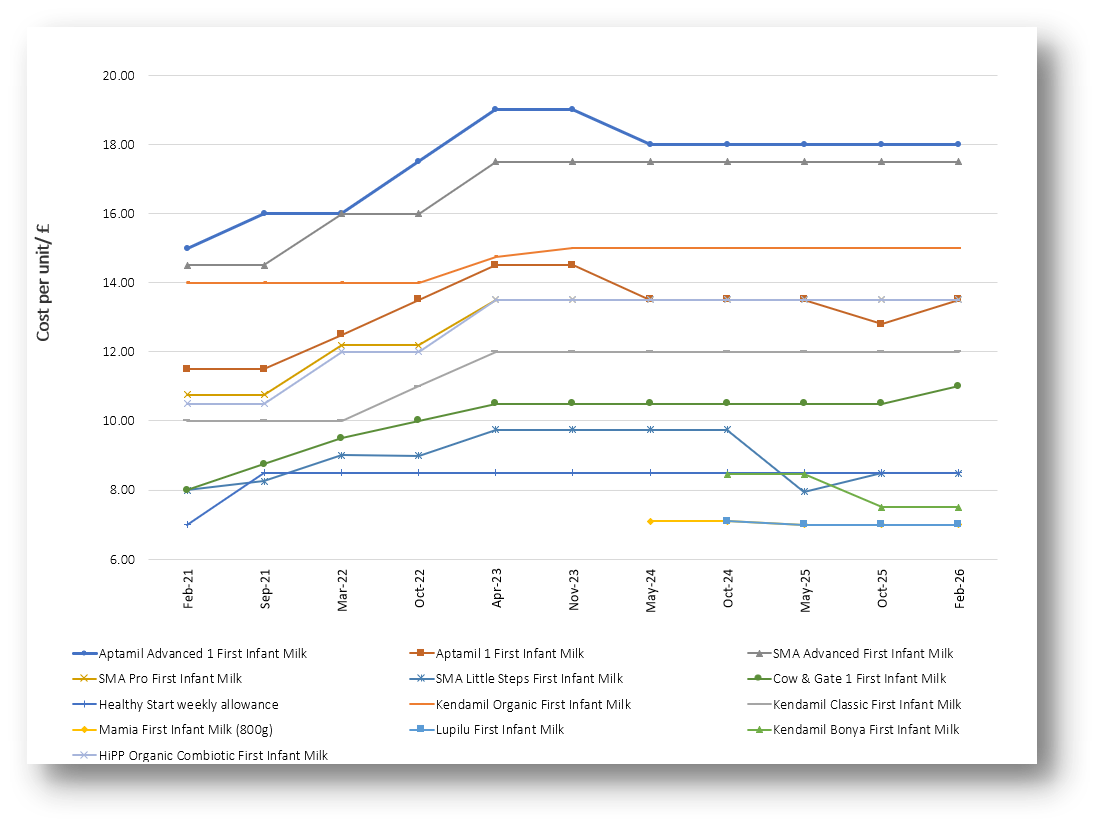
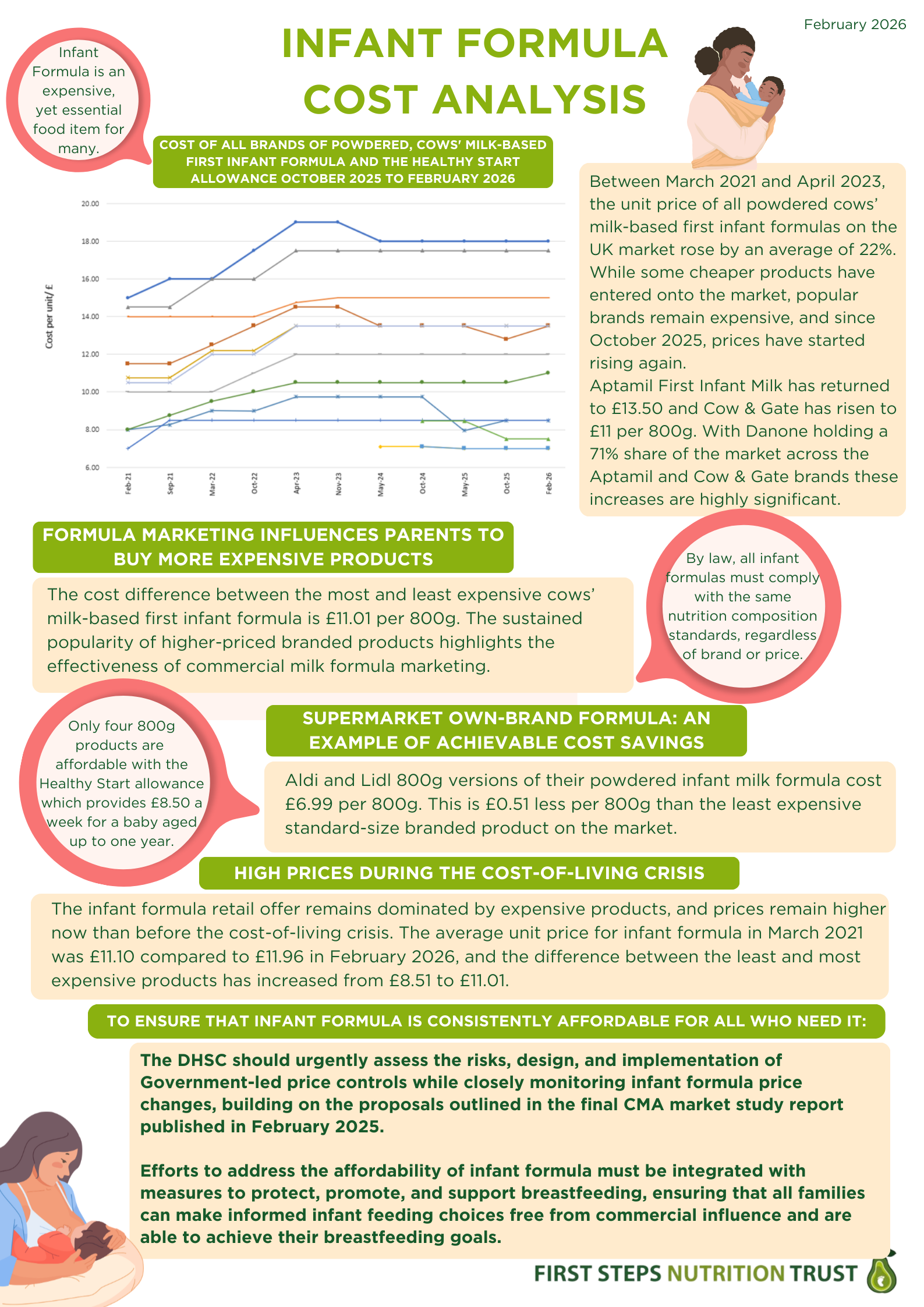
Since October 2025, prices have increased across several major brands, particularly those owned by Danone (Aptamil and Cow & Gate) and Nestlé (SMA), which were affected by the recall (see Graph 1). The average cost of branded powdered first infant formula now stands at £12.95 per 800g tin (6p higher than in October) compared with £6.99 for supermarket own-brand products. Notably, Aptamil First Infant Milk has risen back to £13.50, undoing its earlier price reduction and Cow & Gate has increased to £11 per 800g, its highest recorded price since our monitoring began in March 2021. Although only a small number of products have risen in price, Danone and Nestlé together account for around 85% of the market, making these price increases significant.
Graph 1. Unit cost of powdered, cows' milk-based first infant formula and the Healthy Start allowance, March 2021 to February 2026
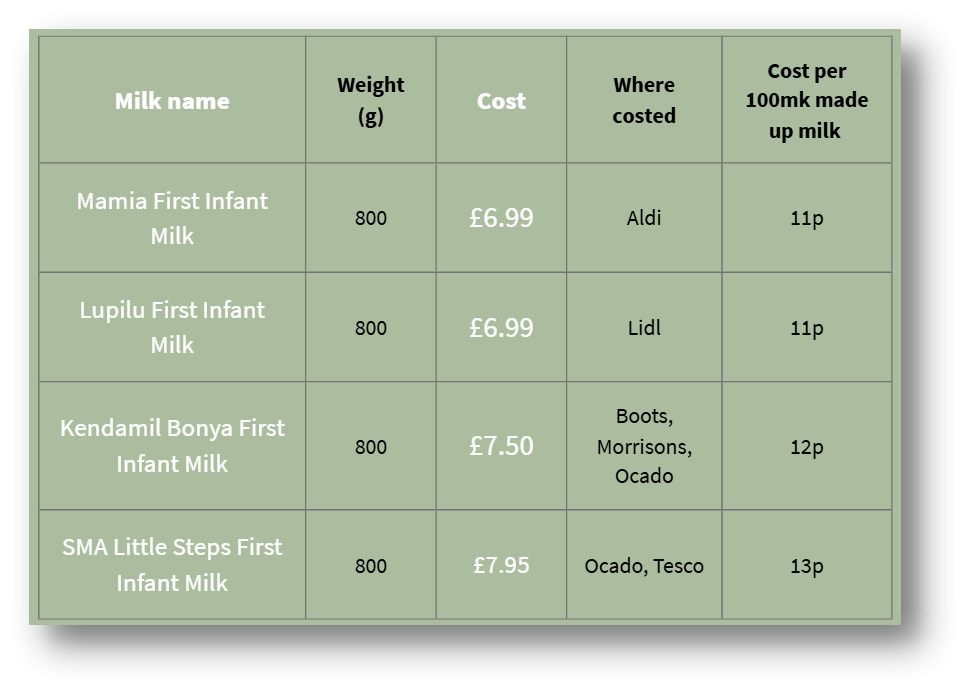
Only four of the 12 standard 800g infant formulas available cost less than the current £8.50 weekly Healthy Start allowance for babies under one, a figure unchanged since May 2025 (see Table 1). Two of these are supermarket own-brand products, which are typically less widely available. Although the allowance will rise to £9.30 in April 2026, this will still not increase the number of full-size tins families can afford at current prices.
Table 1. Lowest cost standard size (800g) infant formula on the UK market in February 2026
Furthermore, larger 2 x 600g packs of Aptamil, Cow & Gate and SMA Pro First Infant Formula, previously seen as more cost-effective purchasing options, have increased by between 50p and £2.65 since October 2025, reducing the value of these bulk-buy options. For example, exclusively formula feeding a 10-week-old baby with two large packs of Cow & Gate First Infant Milk now costs £41.40 per week, up from £36 in October.
Our analysis found that prices for products marketed as specialised milks are rising placing significant financial pressure on families; both those with a baby with a diagnosed clinical need and those influenced by misleading marketing in a weakly regulated market. It’s important to remember that some formulas marketed as specialised milks lack evidence of effectiveness (i.e. comfort milks and hungry milks) while others are recommended in clinical guidelines (i.e. anti-reflux and lactose-free) but should only be used under medical supervision. Specialised formula should only be used following formal diagnosis and on the advice of a healthcare professional, with appropriate clinical supervision and ongoing review.
Prices of ready to feed starter pack of infant formula prices fell between October 2025 and February 2026, likely reflecting the recent Government recommendation that healthcare settings provide infant formula that is competitively priced on the retail market. However, and importantly, these lower upfront prices do not necessarily translate into lower long-term costs. Manufacturers may price starter packs competitively to encourage brand loyalty, while charging more for the equivalent powdered formula used longer term.
Pricing strategies continue to mislead parents into perceiving expensive formulas as superior. The gap between the cheapest and most expensive 800g tin has widened to £11.01 (from £8.51 in March 2021), with prices now ranging from £6.99 to £18. Despite this variation, by law, all infant formulas must meet the same nutritional composition standards, regardless of brand or price and parents can be reassured that it is safe to switch between first infant formula brands.
Adding further complexity for families, retail prices for identical products remain inconsistent across supermarkets, with the retailers offering the lowest prices changing over time.
What needs to happen next
Our findings highlight the financial strain and uncertainty facing families who rely on formula to feed their babies. High and variable pricing, combined with misleading marketing strategies, risks undermining informed decision-making and may contribute to unsafe feeding practices.
In its final market study report published in February 2025, the Competition and Markets Authority proposed that price caps could act as a backstop measure to prevent excessive pricing, although it stopped short of recommending immediate implementation. We therefore strongly urge the Government to assess urgently the risks, design and implementation of potential price controls, so they are ready to act if prices remain high or continue to rise.
Action on formula affordability must sit alongside measures to protect, promote and support breastfeeding. All families should be able to make informed infant feeding decisions, free from commercial influence, and all women should be supported to meet their breastfeeding goals.
Further resources
Below are our two updated infographics, which can be found here on our website. ‘Infant formula cost analysis’ summarises the price trends and our asks of policy makers. ‘Lowest cost infant formula’ shows just that, and is intended to inform parents using formula to feed their babies if they are struggling with the cost.
Update: UK formula milk recalls
As highlighted in our February newsletter, the Food Standards Agency (FSA) issued alerts earlier this year regarding several formula milk products that were contaminated, or potentially contaminated, with the toxin cereulide, which can cause rapid-onset symptoms including nausea, vomiting, diarrhoea and abdominal cramps.
Health care practitioners should continue to advise parents who use formula to feed their babies to check for affected batches and avoid using any recalled products. Comprehensive recall lists, including pack sizes and best-before dates, as well as guidance for professionals, are available here.
Practitioners should also reinforce that powdered infant formula is not sterile. Parents and carers should be encouraged to carefully follow NHS guidance when preparing feeds. A key part of this guidance is using water that has been boiled and then allowed to cool to no less than 70°C before mixing with the powder, as this helps to kill any bacteria that may be present.
Our February formula cost analysis (reported above) identified a significant impact on formula milk availability following the recall. Several supermarkets temporarily withdrew affected Danone (Aptamil and Cow & Gate) and Nestlé (SMA) products, restricting families’ options. At the height of disruption, the Grocer, reported out-of-stocks of 28.4% (98 of 335 products).
Although supply has since improved, many families experienced difficulties. In response, we developed an infographic to support parents and carers, struggling to access their usual formula, available here.
Infant formula remains a necessary and appropriate option for some infants. It is therefore essential that the UK Government takes all necessary steps to ensure product safety and protect the health of vulnerable babies. We are convening with peers to assess this evolving and complex situation and have reached out to the Food Standards Agency to clarify the actions being taken to protect infant health.
For infant milk information please visit our website www.infantmilkinfo.org. If you can’t find what you’re looking for please email rachel@firststepsnutrition.org
Baby Feeding Law Group news
BFLG-UK statement on the Governments’ joint response to the CMA recommendations, and an update on DHSC progress and implementation
As shared previously in our February newsletter, on 3 December 2025, the Government published its joint response to the Competition and Markets Authority (CMA) infant and follow-on formula market study. On 19 February 2026, we published our BFLG-UK statement on this joint response.
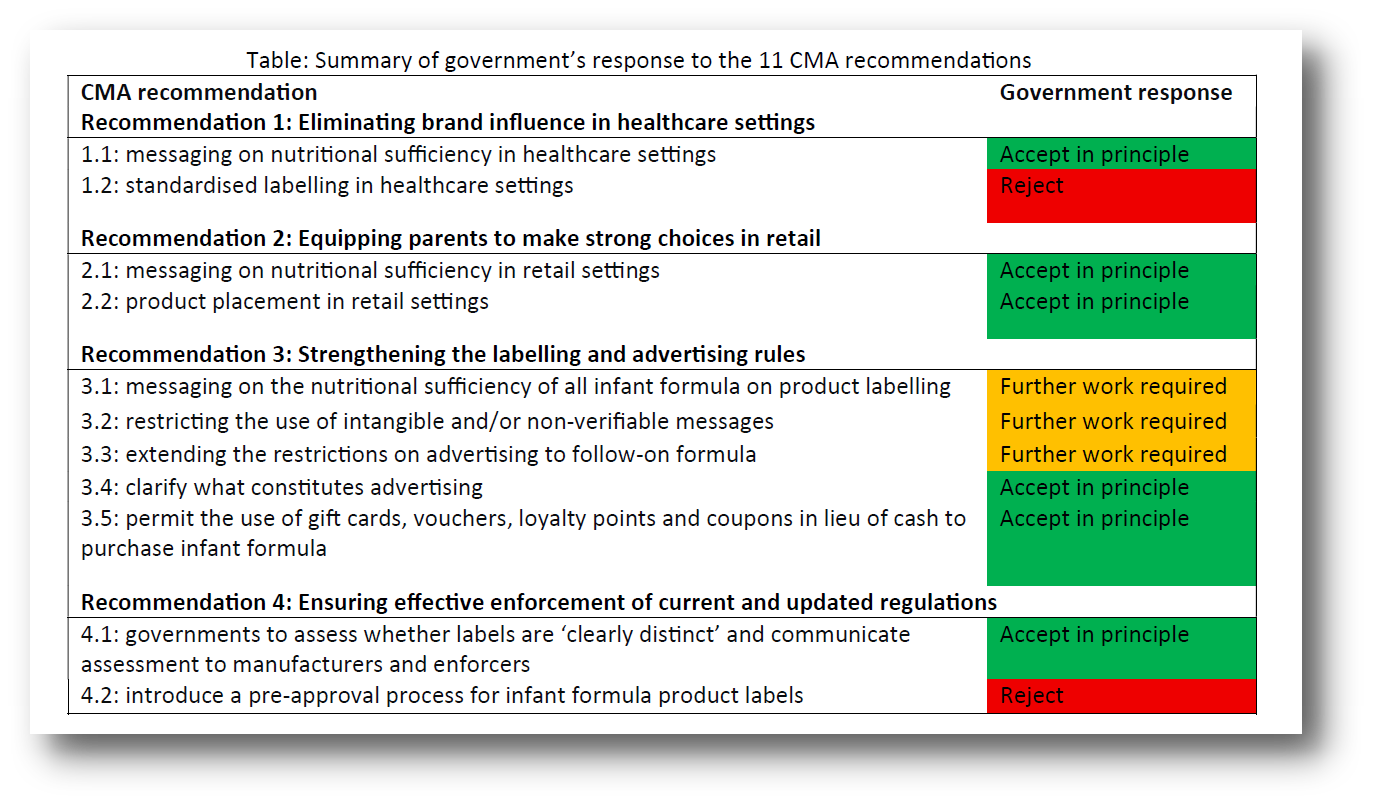
We welcome the government’s acknowledgement of the significant, longstanding issues within the formula market in the UK related to marketing, pricing and retail practices which undermine public health recommendations on infant feeding. The government response makes several notable, positive commitments but further actions will be needed in the short term to deliver significant positive impacts for families and babies, especially those on low incomes. From the 11 recommendations made by the CMA, the government accepted six “in principle”, committed to “further work” on three, and rejected two:
The BFLG-UK statement outlines the steps we welcome and support; steps where greater ambition and urgency is required by the government and what we feel needs to happen next:
We welcome and support:
1. The government commitment to supporting babies, new parents and carers to eat well.
2. The government focus on supporting more informed choices by parent (recommendations 1.1, 2.1).
3. The government’s commitment to clarify what constitutes advertising (recommendation 3.4).
4. The government’s commitment to ensure labelling complies with the law (recommendation 4.1).
Where greater ambition and urgency by the government is required:
1. Strengthening formula labelling and advertising rules (recommendations 3.1, 3.2 and 3.3)
2. Ensuring effective enforcement (recommendation 4.2)
3. Eliminating brand influence in health care settings (recommendation 1.2)
4. Monitoring and intervening to bring down the cost of infant formula (backstop recommendation)
What needs to happen next:
Timely implementation of the 6 CMA recommendations which have been accepted in principle. We have requested more information on the specific actions and timeframes to achieve the above, as well as the indicators which will be used to chart progress and impact. This will then determine when and whether further steps are required.
Clarification on the next steps to strengthen labelling and advertising rules, with a clear timeline for the 3 recommendations (3.1, 3.2 and 3.3) for which further work is required and how this further work will be conducted. The goal should be stronger regulations in line with ‘the Code’, which places restrictions on the advertising of all formula milks marketed for use up to 3 years of age, and their proper enforcement. This would put children’s wellbeing above commercial interests.
Active monitoring and reporting on infant formula prices and commitment to undertaking a formal assessment of the need for and feasibility of implementing more direct measures to improve formula affordability such as profit caps (see above).
We have communicated with the government (including the DHSC and devolved nations) our willingness to support, to ensure that every family has access to affordable products and services they need to ensure the best start in life for their child – and that they are protected from insidious marketing practices that skew feeding choices.
We have met with a representative from the DHSC, and they have shared that they are prioritising delivery of actions, especially those committed to in the government’s manifesto. The DHSC also shared how they are addressing the steps required to implement the government response in their perceived order of priority, including how they are working with and delegating responsibilities to the devolved nations (Food Standards Agency Northern Ireland, Food Standards Scotland and Public Health Wales) and other stakeholders involved in the actions required (for example, the NHS supply chain).
Considering our most recent infant formula costs and trends analyses which show increases (see above), we remain concerned that current actions are insufficient to ensure that infant formula is consistently affordable for parents and families. We therefore continue to advocate for the DHSC to urgently assess the risks, design and implementation of Government-led price controls while closely monitoring infant formula price changes, building on the proposals outlines in the final CMA market study report of February 2025.
For more information about the BFLG-UK please visit our website Baby Feeding Law Group UK (bflg-uk.org) and sign up to our twitter (X) account @BflgUk. You can also email katie@firststepsnutrition.org
Forthcoming
First Steps Nutrition Trust 2025 impact report
We’ve been busy writing our 2025 impact report and have created this infographic below which provides a snapshot of our top achievements of last year. The full report will be available next month. A huge thank you to our generous donors without which our work would not be possible. We are working hard to secure sustainable and more diverse income sources to secure the future of First Steps Nutrition, so please be in touch if you think you can help.
Imperial Ultra-Processed Food Policy Forum, hybrid, March 24th
Following up from 2024’s popular event, the team at Imperial College are hosting another one day UPF food policy forum, assessing the science and advancing regulatory and policy responses to ultra-processed foods. The event convenes world-leading scientists, politicians, policymakers and civil society representatives (including our Director, Vicky) at Imperial College London. Together, they will discuss the latest scientific evidence on UPFs and explore the scope for effective, evidence-based regulatory and policy responses to their growing dominance in people’s diets and their impacts on health.
This year’s Forum will focus on accelerating progress towards a more robust, science-based policy agenda. As governments worldwide intensify efforts to address the expanding role of UPFs in diets, high-quality research is increasingly central to shaping policies that are both effective and sustainable.
Momentum for action in the UK and internationally has continued since the 2024 Imperial event. A series of papers published in The Lancet in November 2025 marked a turning point, providing a strong framework for bridging science and policy (read more in our December newsletter).
The Ultra-processed Food Policy Forum will showcase policy approaches from across the globe, providing policymakers, researchers and civil society with comparative insights and practical lessons for future action. Vicky’s presentation will focus on early years nutrition.
Find out more and register to attend HERE.
An update of First Steps’ Eating Well Healthy Start and Best Start Foods, a practical guide
Next month will see a small but welcome 10% increase in the monetary allowance provided to Healthy Start beneficiaries. To ensure our Eating Well resource Healthy Start and Best Start Foods – A practical guide remains current we will be updating this resource to reflect this increase and other changes in public health recommendations and the wider context since 2022. We will also be sharing new ‘bite sized’ resources, likely including posters, leaflets and recipe cards for use in Family Hubs and food bank settings. Watch out for these new resources in our future newsletters.
The iHV Evidence Based Practice conference, Bournemouth, May 6th
The Institute of Health Visiting (iHV) will be hosting a full-day Evidence-based Practice Conference 2026, with the theme “From Evidence to Action: Getting it right from the start”, at Bournemouth International Centre on Wednesday 6 May 2026. Our Director, Vicky will be doing an oral presentation on Starting solids and the latest public health recommendations on shop bought baby foods. You can book your tickets here before this Saturday, March 7th.
HR News
Welcoming Sara
We’re excited to welcome recently qualified dietitian and MSc Nutrition graduate Sara Esser on to our team as our new Nutritionist. Sara brings with her several years of experience working in public health nutrition with the UCL Healthy Weight Policy Research team. Through her dietetic placements in NHS paediatric settings and her voluntary work supporting vulnerable families, she saw first‑hand the importance of addressing health inequalities to improve early years nutrition and long‑term health, which drew her to working for First Steps. She has particular interests in infant and young child nutrition, the regulation and marketing of breastmilk substitutes, and translating complex guidance into clear, practical information for families and practitioners.